CONTACT US

Minimally Invasive Skin Resurfacing a"Micro Peel", with the SLT Erbium Laser, Thermal Mode and Fractional Mode
Constantin Confino, M.D., Dermatologist, Israel
Betty Czajkowsky, M.D., Sharplight Medical Advisor, Israel
Introduction
Patients and physicians are constantly looking for less invasive techniques to eliminate rhytides and improve skin texture. For more than 15 years ablative lasers (CO2 and Er: YAG ) have been successfully used for the treatment of wrinkles and scars however their widespread use has been limited by the associated down time and the relatively high risk of complications. Non-ablative techniques which are free of these side effects are often preferred even at the expense of clinical efficacy.
Newer types of Er: YAG lasers which employ lower fluencies, thermal modes and fractional beams now offer an alternative which is both minimally invasive and effective. They allow precise tissue ablation with limited residual thermal damage which results in fast re-epithelialization and significantly improved side effect profile.
These new Er: YAG lasers are particularly advantageous for superficial skin ablation, removing from as little as 15-20 microns of tissue, the equivalent of microdermabrasion, and up to the full epidermis. The procedure results in minimal, transient erythema, very fast healing and no downtime. It is highly effective for rejuvenation of the face, neck, chest and hands on both light and dark skin patients, eliminating mild to moderate wrinkles, dyschromias and other signs of aged, photo damaged skin. Using a small spot size with higher fluencies this laser is also effective for the smoothing of acne scars.
Tissue ablation threshold for the Erbium laser is 1-1.5 J/cm2. By adjusting spot size and energy, fluencies above or below this threshold may be set allowing control over amount of tissue ablated and amount of thermal effect.
Erbium microlaserpeel is ideal for a partial to full epidermal peel, is faster and more controlled than chemical peelings and is much deeper than micro dermabrasion. It is easy to apply, safe, has an extremely low complication rate and results in immediate visible improvement. The procedure is repeated at 1-month intervals, 3-4 times, until satisfactory outcome is achieved. A touch-up procedure may be performed every 6 months. Furthermore it may be combined with other facial rejuvenation techniques.
Materials and Methods
The new SLT Erbium laser emits up to 3 pulsesper second at energy per pulse of 0.2-1.2 Joules. Pulse duration is adjustable from 0.3-1.5 msec and spot size may be set at 3 or 6 mm for skin resurfacing, or 1 mm for treatment acne scars. The beam may be delivered in a fractional mode with 49 (7×7) or 81 (9×9) dots. External skin cooling and topical anesthesia are optional.
The laser was used to treat rhytides and other signs of aging skin in 15 patients, 11 females and 4 males, average age 35 to 55 years old. Two treatments were applied 2 months apart. Half of the patients were treated with the regular beam delivery mode and half with the fractional mode. Patients were followed-up at 1 and 3 months post-treatment. Photographs were taken before and at each follow-up visit. All procedures were performed without anesthesia and without any external skin cooling. Eyes were protected with eye shields. At each treatment, the entire treatment area was irradiated with 3 consecutive laser passes with minimal overlap. No wiping was performed between the passes. Additional passes over the wrinkles or scars were applied until the clinical endpoint of skin whitening was obtained. The number of passes needed to reach skin whitening depended on the humidity of the skin and coincides with thermally induced necrosis of the stratum corneum and the epidermis. Normally, more than 3 passes were necessary over wrinkle areas. Fractional pulse mode was used in the same way and under the same conditions.
Results
| Rhytides | Excellent | Good | Fair | No improvement |
| 1 month | 30% | 30% | 30% | 10% |
| 2 months | 50% | 40% | 10% | 0% |
| 3 month | 70% | 25% | 5% | 0% |
No downtime was required in any of the cases. Pinkish to red skin color was observed for the first 24-48 hours. There was no bleeding/oozing or weeping. Dry peel occurred around 7 days afterwards. Total healing time was maximum 10 days. There were no wounds/scars to heal and no demarcation line was observed. Patients could apply make-up and moisturizer the day after the procedure.
Intra- and post-operative discomfort was described as mild by all the patients. First session was performed at lowest energy and largest spot. Energy was increased in subsequent sessions. Treatment area was covered with minimally
overlapping laser pulses. On areas where second pass is performed desiccated tissue debris may first be wiped away with saline soaked gauze, or may be left in place. Skin area should be dry before laser is applied.
Secondary effects like redness and swelling were mild and transient in all the patients. Recovery was quick with minimal post-op complications. Immediate results were visible while collagen renewal is expected to continue for several months post last treatment.
In some patients, discomfort such as after sunburn,was felt for 24 hours. Side effects such as skin over reaction or burning sensation occurred in 2 cases but did not need any special treatment and did not leave any scars. In such cases cold compresses, ointments or water-based moisturizers may be used on the wound. Antiviral medication should be prescribed to patients with history of herpes in the treated area. Long term sun avoidance and protection is recommended.
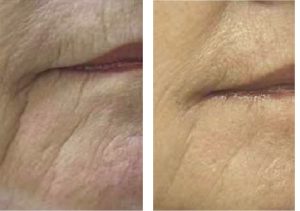
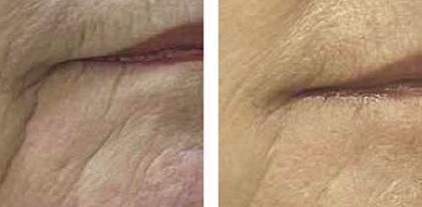
Skin resurfacing one month after 1 thermal mode treatment
Before After 1 treatment
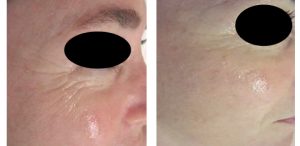
Skin resurfacing one month after 2 thermalA�mode treatments
Before After 2 treatment
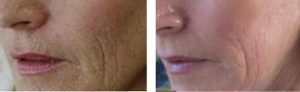
Skin resurfacing one month after 2 fractionalA�mode treatments
Before After 2 fractional treatments
Conclusions
The goal of our study was to determine whether the new SLT Er: YAG laser used with a regular beam mode or a fractional mode is safe and effective for microlaserpeel as previously reported in the literature with other Erbium:YAG lasers. Our study resulted in both patients' and practitioner's satisfaction grade of 95%, with no downtime and no complications. This new laser offers practitioners the flexibility to modify fluencies, spot size, and pulse duration and beam delivery mode thus optimizing treatment parameters to each patient specific clinical need. Clinical results are visible immediately following treatment however full results become evident once all treatment sessions are completed and new collagen synthesis occurs.
References
1. Airan LE, Hruza G. Current lasers in skin resurfacing. Facial Plast Surg Clin North Am 2002;10(1):87-101.
2. Fitzpatrick RE. CO2 laser resurfacing. Dermatol Clin2001;19(3):443-451.
3. Fitzpatrick RE. Maximizing benefits and minimizing risk with CO2 laser resurfacing. Dermatol Clin 2002;20(1):77-86.
4. Alster TS, Lupton JR. Erbium:YAG cutaneous laser resurfacing. Dermatol Clin 2001;19(3):453-466.
5. Sapijaszko MJ, Zachary CB. Er:YAG laser skin resurfacing. Dermatol Clin 2002;20(1):87-96.
6. Berwald C, Levy JL, Magalon G. Complications of the resurfacing laser: Retrospective study of 749 patients. Ann Chir Plast Esthet 2004;49(4):360-365.
7. Grema H, Raulin C, Greve B. "Skin rejuvenation" durch nichtablative Laser- und Lichtsysteme. Literaturrecherche und UA? bersicht. Hautarzt 2002;53(6):385-392.
8. Sadick NS. Update on non-ablative light therapy for rejuvenation: A review. Lasers Surg Med 2003;32:120-128.
9. Williams EF III, Dahiya R. Review of nonablative laser resurfacing modalities. Facial Plast Surg Clin North Am2004;12(3):305-310.
10. Grema H, Greve B, Raulin C. Facial rhytides-subsurfacing or resurfacing? A review. Lasers Surg Med 2003;32(5):405-412.
11. Bjerring P. Photorejuvenationa- An overview. Med Laser Appl 2004;19:186 -195.
12. Ross EV, Barnette DJ, Glatter RD, Grevelink JM. Effects of overlap and pass number in CO2 laser skin resurfacing: A study of residual thermal damage, cell death, and wound healing. Lasers Surg Med 1999;24(2):103-112.
13. Ross EV, McKinlay JR, Sajben FP, Miller CH, Barnette DJ, Meehan KJ, Chhieng NP, Deavers MJ, Zelickson BD. Use of a novel erbium laser in a Yucatan minipig: A study of residual thermal damage, ablation, and wound healing as a function of pulse duration. Lasers Surg Med 2002;30(2):93-100.
14. Majaron B, Srinivas SM, Huang H, Nelson JS. Deep coagulation of dermal collagen with repetitive Er:YAG laser irradiation. Lasers Surg Med 2000;26(2):215-222.
15. Majaron B, Verkruysse W, Kelly KM, Nelson JS. Er:YAG laser skin resurfacing using repetitive long-pulse exposure and cryogen spray cooling: II. Theoretical analysis. Lasers Surg Med 2001 ;28(2):131-137.
16. Kao B, Kelly KM, Majaron B, Nelson JS. Novel model for evaluation of epidermal preservation and dermal collagen remodeling following photorejuvenation of human skin. Lasers Surg Med 2003;32(2):115-119.
17. Drnovsek-Olup B, Beltram M, Pizem J. Novel model for evaluation of epidermal preservation and dermal collagen remodeling following photorejuvenation of human skin. Lasers Surg Med 2003;32(2):115-119.
18. Ross EV, Miller C, Meehan K, McKinlay J, Sajben P, Trafeli JP, Barnette DJ. One-pass CO2 versus multiple-pass Er:YAG laser resurfacing in the treatment of rhytides: A comparison side-by-side study of pulsed CO2 and Er:YAG lasers. Dermatol Surg 2001;27(8):709-715
19. Adrian RM. Pulsed carbon dioxide and long pulse 10-ms erbium-YAG laser resurfacing: A comparative clinical and histologic study. J Cutan Laser Ther 1999;1(4):197-202.
20. Newman JB, Lord JL, Ash K, McDaniel DH. Variable pulse erbium:YAG laser skin resurfacing of perioral rhytides and side-by-side comparison with carbon dioxide laser. Lasers Surg Med 2000;26(2):208-214.
21. Drosner M. Non-ablative wrinkle reduction by Er:YAG laser: Encouraging results (case report). Lasers Surg Med 2002; Suppl 14:66.
22. Kunzi-Rapp K, Cambier B, Drosner M, Dierickx C, Levy JL, Russ D, Steiner R. Non-ablative skin rejuvenation with Erbium:YAG laser pulses – investigation of structural changes in the skin. Lasers Med Sci 2003;18(Suppl 1):1-68.
23. Kunzi-Rapp K, Cambier B, Drosner M, Dierickx C, Levy JL, Larrouy JC, Russ D, Steiner R. Nonablative versus ablative Er:YAG laser therapy in photoaged skin: Histopathological changes. Lasers Surg Med 2004; Suppl 16:21.
24. Drnovsek-Olup B, Beltram M, Pizem J. Repetitive Er:YAG laser irradiation of human skin: A histological evaluation. Lasers Surg Med 2004;35:146-151.
25. Trelles MA, Allones I, Luna R. Facial rejuvenation with a nonablative 1320 nm Nd:YAG laser: A preliminary clinical and histologic evaluation. Dermatol Surg 2001;27(2):111-116.
26. Maneker GM, Wrone DA, WilliamRM, Moy RL. Treatment of facial rhytides with a non-ablative laser; a clinical and histologic study. Dermatol Surg 1999;25:440-444.
27. Stuzin JM, Baker TJ, Baker TM, Kligman AM. Histologic effects of the high-energy pulsed CO2 laser on photoaged facial skin. Plast Reconstr Surg 1997;99(7):2036-
28. Kligman AM, Zheng P, Lavker RM. The anatomy and pathogenesis of wrinkles. Br J Dermatol 1985;113(1):37-42.
29. Fisher GJ, Kang S, Varani J, Bata-Csorgo Z, Wan Y, Datta S, Voorhees JJ. Mechanisms of photoaging and chronological skin aging. Arch Dermatol 2002;138(11):1462-1670.
30. El-Domyati M, Attia S, Saleh F, Brown D, Birk DE, Gasparro F, Ahmad H, Uitto J. Intrinsic aging vs. photoaging: A comparative histopathological, immunohistochemical, and ultrastructural study of skin. Exp Dermatol 2002;11(5):